There are two types of diabetes: type 1 diabetes, which usually occurs in childhood or adolescence and is also known of as juvenile diabetes, and type 2 diabetes.
With type 1 diabetes, the body stops producing insulin, the hormone that usually stimulates the body’s cells to uptake glucose from the blood to use for energy. This lack of insulin necessitates external administration of the hormone, which is why the condition is also known of as Insulin-dependent Diabetes Mellitus (IDDM).
Type 2 diabetes is a chronic condition that affects millions of people worldwide. Around 75% of people with diabetes have type 2 diabetes mellitus. This has also been called Non-Insulin Dependent Diabetes Mellitus (NIDDM) or maturity-onset Diabetes Mellitus. In type 2 diabetes, the body does not produce enough insulin or the insulin that is made by the body does not exert the usual effects on body cells. The incidence of type 2 diabetes is on the rise worldwide as the number of health problems increases.
Understanding Type 2 Diabetes is important for individuals who are at risk or have been diagnosed with the condition. Symptoms of Type 2 Diabetes can include increased thirst, frequent urination, blurred vision, and fatigue. Early detection is key to managing the condition and preventing complications.
Treatment and Management of Type 2 Diabetes can include lifestyle changes such as diet and exercise, as well as medications and insulin therapy. It is important for individuals with Type 2 Diabetes to work closely with their healthcare team to develop a personalized treatment plan. In this article, we will explore everything you need to know about Type 2 Diabetes, from symptoms and early detection to treatment and management.
Key Takeaways
- Type 2 Diabetes is a chronic condition that occurs when the body becomes resistant to insulin or does not produce enough of it, leading to high blood sugar levels.
- Early detection of Type 2 Diabetes is key to managing the condition and preventing complications.
- Treatment and Management of Type 2 Diabetes can include lifestyle changes such as diet and exercise, as well as medications and insulin therapy.
The Role of Insulin and Glucose
IN THIS ARTICLE
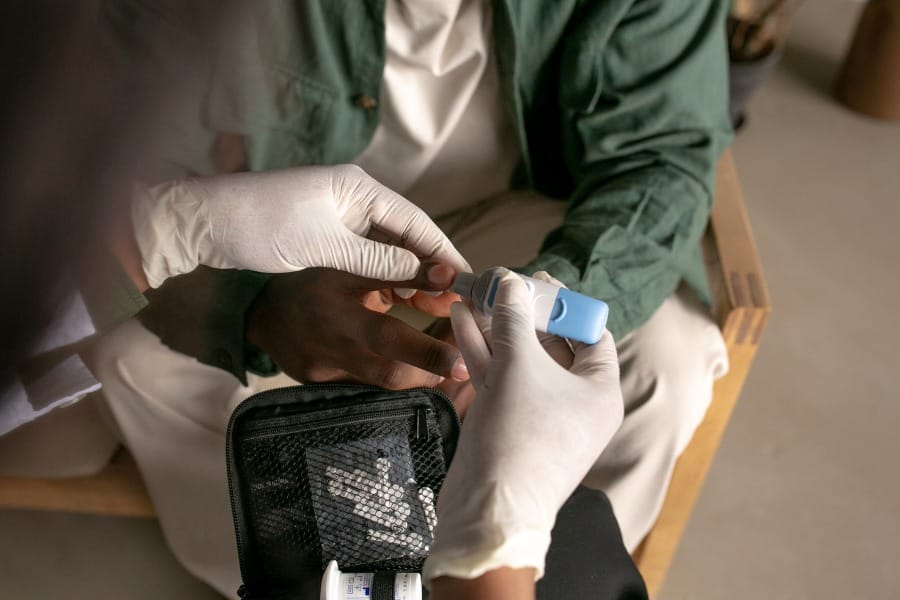
Insulin is a hormone produced by the pancreas that helps regulate blood sugar levels in the body. After eating, the body breaks down carbohydrates into glucose, which enters the bloodstream. Insulin then helps move glucose from the bloodstream into cells where it can be used for energy.
In people with type 2 diabetes, the body becomes resistant to insulin, which means that the cells do not respond to insulin as they should. This results in high blood sugar levels, which can lead to a range of health problems.
Diabetes vs. Prediabetes and Gestational Diabetes
Prediabetes is a condition in which blood sugar levels are higher than normal but not high enough to be diagnosed as type 2 diabetes. People with prediabetes are at an increased risk of developing type 2 diabetes, but the condition can often be reversed through lifestyle changes. Gestational diabetes is a type of diabetes that occurs during pregnancy.
It usually goes away after the baby is born, but women who have had gestational diabetes are at an increased risk of developing type 2 diabetes later in life.
Essentialy, type 2 diabetes is a chronic condition that affects how the body processes blood sugar. Insulin resistance is a key factor in the development of type 2 diabetes. Risk factors for type 2 diabetes include obesity, physical inactivity, family history of diabetes, high blood pressure, and abnormal cholesterol levels. Lifestyle changes such as losing weight, increasing physical activity, and eating a healthy diet can help prevent or delay the onset of type 2 diabetes.
Prediabetes and gestational diabetes are two related conditions that also affect blood sugar levels and increase the risk of developing type 2 diabetes.
Symptoms of Diabetes
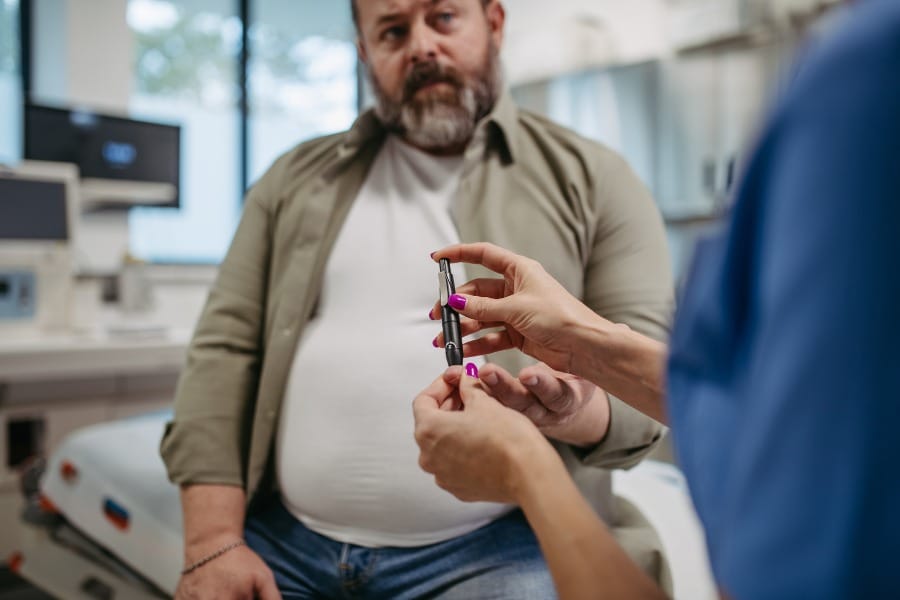
Type 2 diabetes is a chronic condition that affects the way the body processes blood sugar (glucose). It is important to recognize the symptoms of type 2 diabetes early to prevent complications. The symptoms of type 2 diabetes can be subtle and may develop slowly over time. Some of the common symptoms of type 2 diabetes include:
- Urinating often
- Feeling very thirsty
- Feeling very hungry – even though you are eating
- Extreme fatigue
- Blurry vision
- Cuts/bruises that are slow to heal
- Weight loss – even though you are eating more (Type 1)
- Tingling, pain, or numbness in the hands/feet (Type 2)
If you notice any of the above symptoms, contact your primary physician. Although the cause of type 2 diabetes is largely unknown, genetics and lifestyle habits clearly play a role, and the risk of having type 2 diabetes increases as a person gets older.
Importance of Early Diabetes Detection
Early detection of type 2 diabetes is crucial to prevent complications. If left untreated, type 2 diabetes can lead to serious health problems such as heart disease, kidney disease, and nerve damage.
It is recommended that individuals who are at risk for type 2 diabetes get tested regularly. Risk factors for type 2 diabetes include:
- Being overweight or obese
- Having a family history of diabetes
- Being physically inactive
- Having high blood pressure or high cholesterol levels
- Being over the age of 45
Testing for type 2 diabetes involves a blood test to measure blood sugar levels. If you are diagnosed with type 2 diabetes, your healthcare provider will work with you to develop a treatment plan that may include lifestyle changes such as diet and exercise, as well as medication if necessary.
Diabetes Risk Factors
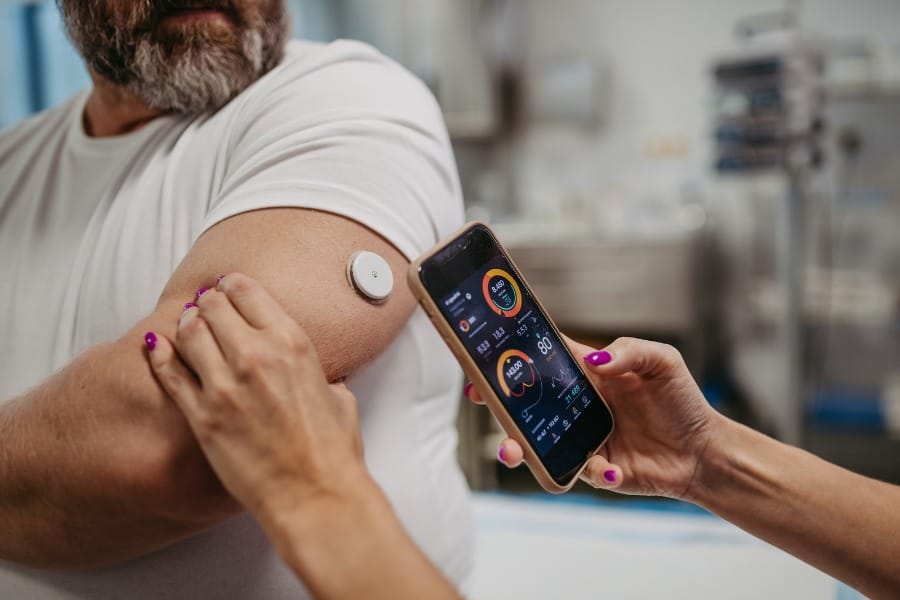
Type 2 diabetes has been linked to obesity, genetic risk factors, and inactivity. Here are some lifestyle factors that can increase the risk of type 2 diabetes:
- Weight: Being overweight is a primary risk factor for type 2 diabetes. The more fatty tissue you have, the more resistant your cells become to insulin. However, you don’t have to be overweight to develop type 2 diabetes.
- Fat distribution: If your body stores fat primarily in your abdomen, your risk of type 2 diabetes is greater than if your body stores fat elsewhere, such as your hips and thighs.
- Inactivity: The less active you are, the greater your risk of type 2 diabetes. Physical activity helps you control your weight, uses up glucose as energy and makes your cells more sensitive to insulin.
- Family history: The risk of type 2 diabetes increases if your parent or sibling has type 2 diabetes.
- Race: Although it’s unclear why, people of certain races — including African Americans, Hispanics, American Indians and Asian-Americans — are more likely to develop type 2 diabetes than caucasians are.
- Age: The risk of type 2 diabetes increases as you get older, especially after age 45. That’s probably because people tend to exercise less, lose muscle mass and gain weight as they age. But type 2 diabetes is also increasing dramatically among children, adolescents, and younger adults.
If you or a loved one is living with diabetes, a private duty nurse can provide wellness checks or care for other skilled needs, all in the comfort of home.
There are many short-term and long-term complications associated with type 2 diabetes, many of which result from the mismanagement of blood sugar levels. A licensed nurse can help improve quality of life for someone diagnosed with diabetes.
Hypoglycemia, or low blood glucose (blood sugar), is one of two major short-term consequences of type 2 diabetes. It is possible for your blood glucose to drop, especially if you’re taking insulin or a sulfonylurea drug, which helps your body produce insulin throughout the day.
Combining these medications with an inadequate amount of food or more activity than usual can cause blood glucose levels to dip too much. Hypoglycemia may also be caused by certain medications (aspirin, for example, lowers the blood glucose level if you take a dose of more than 81mg) and too much alcohol, which keeps the liver from releasing glucose. Symptoms of low blood sugar are easy to recognize:
- Rapid heartbeat
- Sweating
- Whiteness of skin
- Anxiety
- Numbness in fingers, toes, and lips
- Sleepiness
- Confusion
- Headache
- Slurred speech
Mild cases of hypoglycemia can be treated by drinking orange juice or eating a glucose tablet—both will quickly raise your blood glucose level.
If you have type 2 diabetes and you take insulin, you should always carry glucagon with you. If you become unresponsive or unconscious due to hypoglycemia, you will need a quick injection of glucagon, a hormone that starts a process in your body that raises your blood glucose levels.
The second short-term consequence of type 2 diabetes is hyperosmolar hyperglycemic nonketotic syndrome (HHNS). Although it is very rare, it is important to be aware of it and know how to handle it if it occurs.
HHNS occurs when blood glucose levels go extremely high. If left untreated, it can cause death. HHNS is most likely to occur when you’re sick, and elderly people are at a higher risk of developing it. It starts when your blood glucose level starts to climb. When that happens, your body will try to get rid of all the excess glucose through frequent urination. This in turn leads to dehydration, which will cause you to become very thirsty.
Unfortunately, when you’re sick, you can’t always rehydrate your body as well as you should. For example, you might have trouble keeping fluids down. When you don’t rehydrate your body, the blood glucose level continues to climb, and it can eventually go so high that it will send you into a coma.
Short-term consequences of diabetes can post extreme risks to your health, which is why it’s so important to manage your blood glucose levels. Keeping blood glucose at a healthy level will also help protect the body against long-term complications, too.
Diabetes Management

Medication Options
When it comes to managing type 2 diabetes, medication can be an important tool. One of the most commonly prescribed medications for type 2 diabetes is metformin. Metformin works by lowering glucose production in the liver and improving the body’s sensitivity to insulin so it uses insulin more effectively. Some people may experience vitamin B12 deficiency and may need to take supplements.
Other diabetes medications may be prescribed depending on the individual’s needs and situation. It is important to work closely with a healthcare provider to determine the best medication regimen for managing type 2 diabetes.
Lifestyle Modifications
In addition to medication, lifestyle modifications can also play a crucial role in managing type 2 diabetes. Making healthy lifestyle choices, such as eating a balanced diet and engaging in regular physical activity, can help control blood sugar levels and improve overall health.
A healthy diet for individuals with type 2 diabetes typically involves limiting processed and sugary foods and focusing on whole foods, such as fruits, vegetables, and lean proteins. Regular exercise can also help improve blood sugar control and overall health.
Monitoring and Testing
Monitoring blood sugar levels is an important part of managing type 2 diabetes. A glucose meter can be used to measure blood sugar levels at home. Some individuals may also benefit from using a continuous glucose monitor, which provides real-time information about blood sugar levels.
Regular testing of other health markers, such as blood pressure and cholesterol levels, can also be important for managing type 2 diabetes.
Keeping Your Blood Glucose Levels in Check
By keeping your blood glucose level in a healthy range through meal planning, physical activity, and medications, you can avoid long-term complications of diabetes.
These complications develop over many years and all relate to how blood glucose levels can affect blood vessels. Over time, high blood glucose can damage the body’s blood vessels, both tiny and large. Damage to your tiny blood vessels causes microvascular complications; damage to your large vessels causes macrovascular complications.
Microvascular damage is caused by damaged blood vessels, which don’t deliver blood as well as they should. This leads to other problems, especially with the eyes, kidneys, and nerves.
-
- Eyes: Blood glucose levels out of range for a long period of time can cause cataracts and/or retinopathy in the eyes—both can cause vision loss. To avoid eye problems associated with diabetes, keep your blood glucose within range and schedule annual eye exams that include a dilated eye examination with your optometrist.
- Kidneys: If untreated, kidney disease (also called diabetic nephropathy) leads to impaired kidney function, dialysis and/or kidney transplant. Uncontrolled (or poorly controlled) diabetes can cause the kidneys to fail, as they will be unable to clean the blood properly. To prevent diabetic nephropathy, you should be tested every year for microalbuminuria, a condition that’s an early indicator of kidney problems. The test measures how much protein is in the urine and is easily done with a urine sample. When the kidneys begin to have problems, they start to release too much protein. Medications can help prevent further damage, once microalbuminuria is diagnosed.
- Nerves: Nerve damage caused by diabetes is also known as diabetic neuropathy. The tiny blood vessels “feed” your nerves, so if the blood vessels are damaged, then the nerves will eventually be damaged as well. In type 2 diabetes, some people will already show signs of nerve damage when they’re diagnosed. This is an instance where getting the blood glucose levels under control can prevent further damage.There are various forms of diabetic neuropathy: peripheral, autonomic, proximal, and focal. Diabetic peripheral neuropathy is the most common form of nerve damage, and it most often affects the nerves going to the hands and feet. People who have had type 2 diabetes for a very long time and who haven’t done well managing their blood glucose may lose sensation in their feet. They may also experience pain, weakness, or tingling. One serious complication of diabetic peripheral neuropathy in the feet is that people may not realize when they have a sore on their foot. The sore can become infected, the infection can spread, and left untreated, the foot may need to be amputated to keep the infection from spreading more. It is important to have regular foot exams done by a podiatrist, but you should also have your healthcare provider examine your feet every time you have an office visit.
Type 2 diabetes can also affect the large blood vessels, causing plaque to build up over time and increasing the risk of heart attack, stroke or vessel blockage in the legs (peripheral vascular disease). To prevent heart disease and stroke as a result of diabetes, you should manage your diabetes well, but you should also make heart-healthy choices in other areas of your life: don’t smoke, keep your blood pressure under control, and pay attention to your cholesterol.
The total estimated cost of diagnosed diabetes in 2012 was $245 billion, including $176 billion in direct medical costs and $69 billion in reduced productivity. Since then, the costs of diagnosed diabetes have risen to $327 billion in 2017.
The largest components of medical expenditures are:
- Hospital inpatient care (43% of the total medical cost)
- Prescription medications to treat complications of diabetes (18%)
- Anti-diabetic agents and diabetes supplies (12%)
- Physician office visits (9%)
- Nursing/residential facility stays (8%)
People with diagnosed diabetes incur average medical expenditures of about $13,700 per year, of which about $7,900 is attributed to diabetes. People with diagnosed diabetes, on average, have medical expenditures approximately 2.3 times higher than what expenditures would be in the absence of diabetes. For the cost categories analyzed, care for people with diagnosed diabetes accounts for more than 1 in 5 health care dollars in the US, and more than half of that expenditure is directly attributable to diabetes.
Indirect costs include:
- Increased absenteeism ($5 billion)
- Reduced productivity while at work for the employed population ($20.8 billion)
- Reduced productivity for those not in the labor force ($2.7 billion)
- Inability to work as a result of disease-related disability ($21.6 billion)
- Lost productive capacity due to early mortality ($18.5 billion)
Complications and Comorbidities
Type 2 diabetes can lead to a variety of complications and comorbidities, both in the short-term and long-term. Here are some of the most common ones:
Short-Term Complications
Short-term complications of type 2 diabetes can occur when blood sugar levels are too high or too low. These complications can be serious and require immediate medical attention. Some of the short-term complications of type 2 diabetes include:
- Hypoglycemia (low blood sugar)
- Hyperglycemia (high blood sugar)
- Diabetic ketoacidosis (DKA)
- Hyperosmolar hyperglycemic state (HHS)
Long-Term Complications
Long-term complications of type 2 diabetes can develop over time and are often related to damage to blood vessels and nerves. These complications can be serious and can affect many parts of the body. Some of the long-term complications of type 2 diabetes include:
- Heart disease
- Stroke
- Kidney disease
- Nerve damage (neuropathy)
- Eye damage (retinopathy)
- Skin problems
- Erectile dysfunction (ED)
Get a Professional Nurse

Nurses can help diabetic patients by offering a complete range of services to improve their quality of life. Registered Nurses (RNs) provide support by working closely with the physician and evaluating the patient’s needs related to diabetes and any associated conditions.
Nurses can develop a customized care plan according to the patient’s needs. In general, a nursing care plan helps the patient gain control of the disease. Nurses can monitor blood sugar levels, ensure the patient is taking medications as prescribed, assist with insulin injections, and educate the client on lifestyle changes that need to be made.
Nurses can visit regularly, depending on the patient’s needs, and can also help with procuring the medication and other supplies for care. Through these visits, the nurse develops a good understanding of the patient’s health status and is be able to assess the progress of the disease condition accurately. This also allows the nurse to review and revise the care plan accordingly as the patient’s needs change. The nurse can:
- Specifically, assess vitals and blood glucose levels
- Monitor the development of diabetes-related complications, including neuropathy, nephropathy, retinopathy, diabetic foot, and other co-morbid conditions
Additionally, caregivers can provide basic personal care on a continuous basis and help the patient with activities of daily living.
If you or a loved one is living with diabetes, a private duty nurse can provide wellness checks and other skilled care services, all in the comfort of home. Click below to learn more.
Frequently Asked Questions about Diabetes
What are the common symptoms of Type 2 diabetes?
Type 2 diabetes is a chronic disease that affects how your body processes glucose, the main source of energy for your cells. Common symptoms include frequent urination, increased thirst, unexplained weight loss, blurred vision, fatigue, and slow healing of wounds. However, some people with Type 2 diabetes may not show any symptoms at all.
Can Type 2 diabetes be inherited?
Type 2 diabetes can be inherited, but it is not always the case. There are many factors that can increase your risk of developing Type 2 diabetes, including genetics, lifestyle choices, and environmental factors. If you have a family history of Type 2 diabetes, it is important to maintain a healthy lifestyle to reduce your risk of developing the disease.
How is Type 2 diabetes diagnosed?
Type 2 diabetes is diagnosed through a blood test that measures your blood glucose levels. If your blood glucose levels are higher than normal, you may be diagnosed with prediabetes or Type 2 diabetes. Your doctor may also perform other tests to determine if you have any complications related to Type 2 diabetes.
What are the main risk factors for developing Type 2 diabetes?
The main risk factors for developing Type 2 diabetes include being overweight or obese, having a family history of the disease, being physically inactive, having high blood pressure or high cholesterol levels, and being over the age of 45. Other risk factors include a history of gestational diabetes, polycystic ovary syndrome (PCOS), and sleep apnea.
How does Type 2 diabetes affect insulin production and usage in the body?
Type 2 diabetes affects insulin production and usage in the body by reducing the body’s ability to produce insulin or by making the cells in the body more resistant to insulin. Insulin is a hormone that helps regulate blood glucose levels in the body. When the body is unable to produce or use insulin effectively, glucose builds up in the bloodstream, leading to high blood glucose levels.
What lifestyle changes are recommended for managing Type 2 diabetes?
Lifestyle changes are an important part of managing Type 2 diabetes. These include maintaining a healthy weight, eating a balanced diet that is low in sugar and refined carbohydrates, engaging in regular physical activity, monitoring blood glucose levels regularly, taking medication as prescribed, and quitting smoking. It is also important to manage stress levels and get enough sleep to prevent complications related to Type 2 diabetes.
References
Leontis, L., “Type 2 Diabetes Complications,” EndocrineWeb, March 12, 2016.
“Home Health Care and Diabetes Management,” India Home Health Care, September 11, 2014.
Mandal, A., “What is Type 2 Diabetes?” News Medical Life Sciences, January 31, 2014.
“Diabetes Symptoms,” American Diabetic Association, June 1, 2015.
“What Causes Diabetes?” New York State Department of Health, January 2015.
“Types of Diabetes – Symptoms and Causes,” Mayo Clinic, January 13, 2016.
“The Cost of Diabetes,” American Diabetes Association, January 30, 2019.






