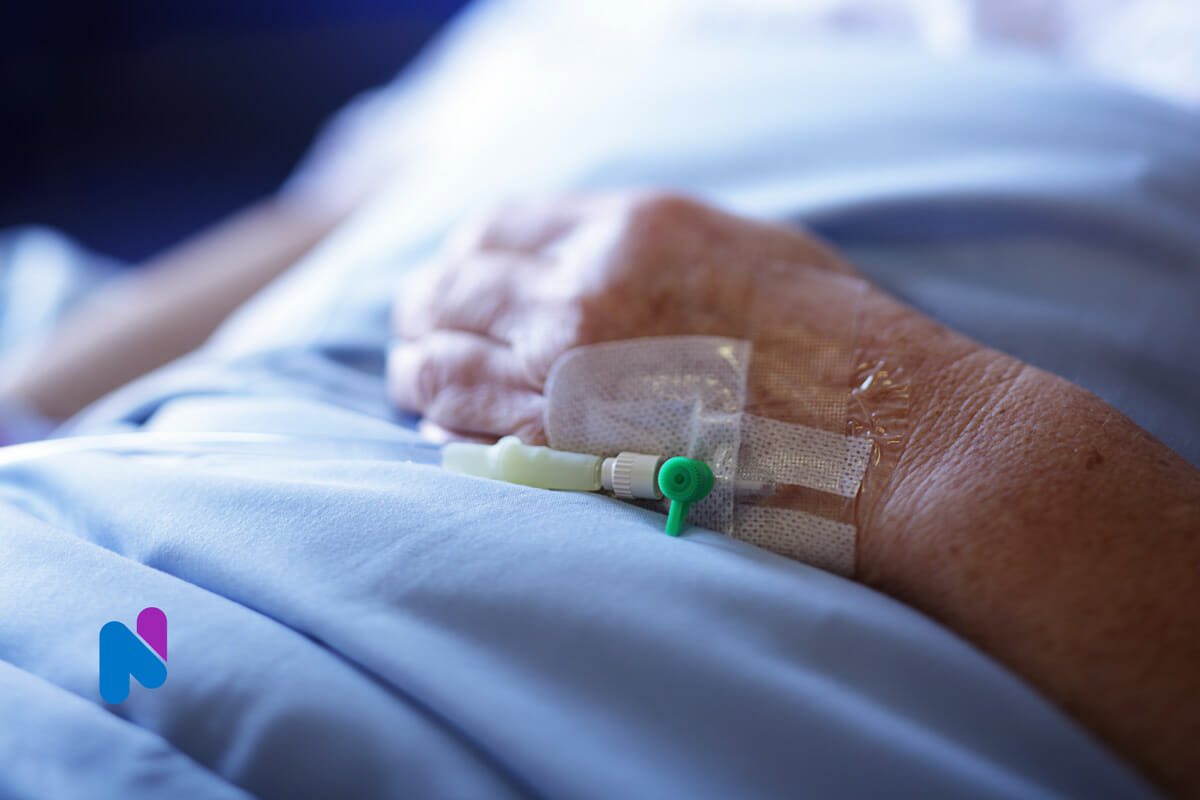
Many hospitals have an intensive care unit (ICU) within their facility.
This is a section of the hospital that requires focus and resilience from the various doctors, nurses, and other healthcare professionals.
They provide high-quality specialty care for patients with serious conditions and illnesses. Individuals may be admitted to the ICU for numerous reasons, such as after a serious accident or major surgery.
Some people may feel a sense of intimidation when admitted due to the large quantity of monitoring equipment, wires, and tubes. Creating an advanced care plan could be valuable for immediate family and the ICU staff.
Key Takeaways:
- The ICU (Intensive Care Unit) is a specialized hospital unit that provides around-the-clock monitoring and life support for patients with life-threatening conditions, serious injuries, or illnesses.
- Patients are admitted to the ICU when they require critical care, such as after major surgery, a serious accident, organ failure, or a severe infection like sepsis.
- The ICU is equipped with advanced medical equipment like ventilators, patient monitors, and infusion pumps to support patients’ vital functions.
- A multidisciplinary team of doctors, specialty nurses, therapists, and other staff provide comprehensive care to ICU patients.
- For planned ICU stays, creating an advance care plan outlining treatment preferences can help guide the medical team if the patient becomes unable to communicate.
What is an ICU?
IN THIS ARTICLE
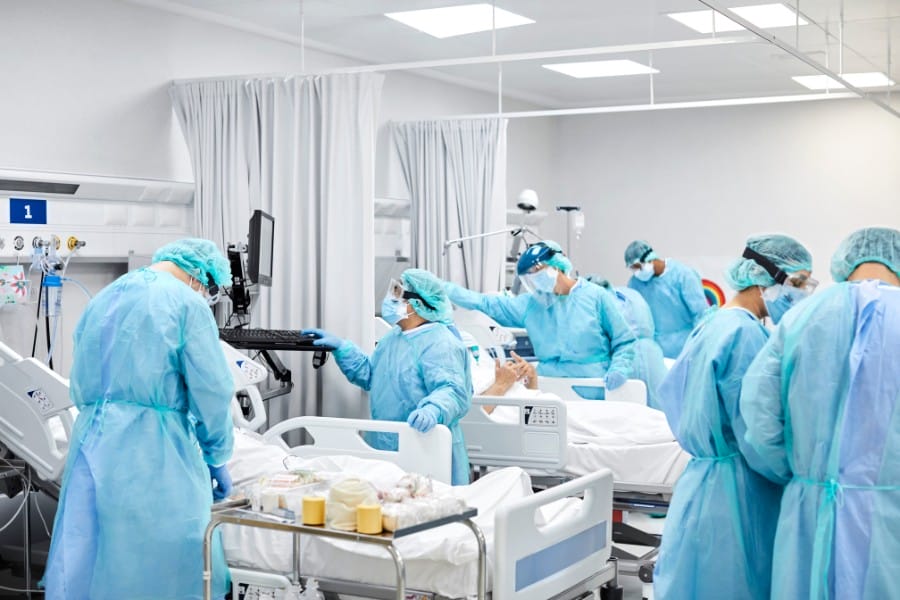
The ICU is the division of the hospital that provides care for patients with life-threatening health conditions like serious injuries, accidents, or illnesses.
Common factors that will determine whether someone is admitted include:
- Illness severity
- Diagnosis
- Availability of treatment
- Anticipated quality of life
- Current response to treatment
Individuals receive 24/7 monitoring and life support, if necessary, from highly skilled specialists.
There is an array of high-quality equipment, including a patient monitor, ventilator, defibrillator, CPAP & BiPAP system, infusion pump, and syringe pump.
Why do individuals get admitted into the ICU?
Someone may be admitted to the ICU because they need critical medical support.
Some patients may be admitted for a failing organ system or a terminal/chronic illness.
Others may be admitted following a major surgery, car accident or intense burn, or when a serious infection arises (like sepsis or pneumonia).
Here is an overview breakdown of why someone may be admitted to ICU rather than a typical emergency room or critical care unit.
- Respiratory arrest
- Cardiac arrest
- A pulse less than 40 or greater than 140 bpm
- Severe and repetitive seizures
- An obstructed airway
What happens in an ICU?
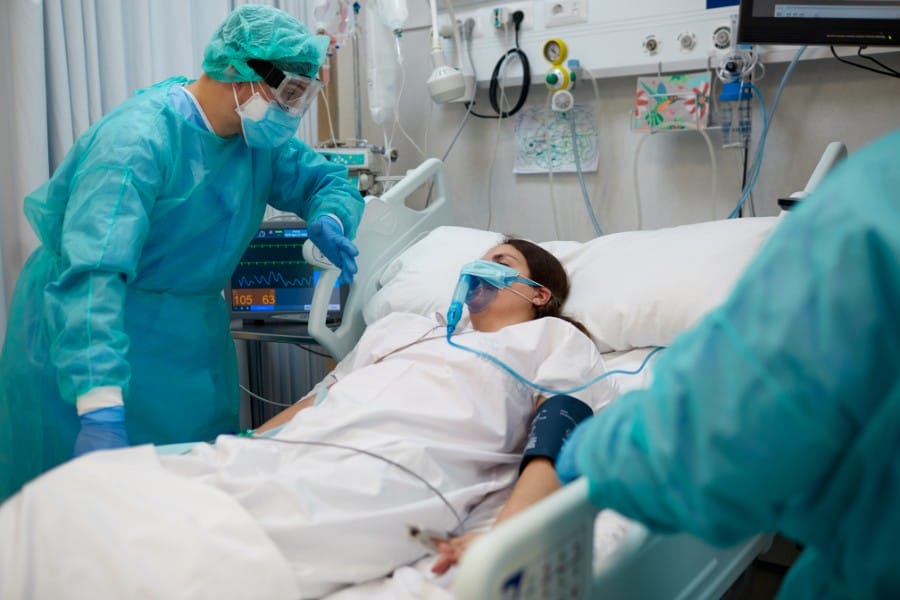
An ICU provides 24-hour patient care for individuals with life-threatening conditions. The ICU can be unnerving for admitted patients and their family or friends.
Often, this nervousness is caused by the life support machines—the many wires, tubes, lines, and loud monitoring equipment in the ICU.
Much of the time, patients will be connected to a large variety of machines, such as a vitals monitor, so staff can pay close attention to them. They may be attached to a ventilator if they have trouble with breathing.
Most ICU machines make loud sounds to alert medical professionals when changes occur in a patient’s condition. Sometimes patients will need several tubes to have fluids removed or for nutrition administration.
Who will you see in the ICU?
The ICU has doctors, specialty nurses, speech therapists, dieticians, and physiotherapists.
Nurses
Typically, one specialty nurse will actively monitor one or two patients at most. They are responsible for the majority of the care that a person will need in the ICU.
These nurses also spend a lot of time with the patients in the early stages of their conditions. Nurses work with doctors and other medical professionals to give the best quality care possible.
Nurses perform many tasks, which include taking regular blood tests or adjusting treatment based on test results.
Doctors
The ICU will typically have a consultant who will lead a team of doctors. They visit each patient and make decisions regarding their treatment.
Doctors spend time examining patients thoroughly and pay close attention to any wounds.
Dieticians
The dietician will provide the medical staff with important advice to manage the nutritional needs of critically ill patients.
They will also determine if a patient needs to be fed through a nasogastric tube or a drip if needed.
Physiotherapists
Patients will be seen by a physiotherapist. They are responsible for making sure the patient’s lungs are clear. They also exercise the patients so their joints won’t get stiff.
Patients will also be given exercises to help strengthen their lungs and breathing muscles.
Speech Therapists
Speech therapists will see patients who have had a tracheostomy to help them breathe. They also offer intensive monitoring to see when they can drink and eat normally again.
How do you prepare for the ICU?

In some cases, ICU admission happens unexpectedly and is hard to prepare for. However, some individuals know they will have to go.
If you or a loved one anticipate an ICU stay, it is a good idea to create an advanced care plan. This can be useful for ICU staff and family members of the patient.
The plan includes the person’s decisions regarding treatment if they are unable to speak or their condition worsens.
Common Medication in ICU
Many ICU patients receive pain relievers or sedatives. These may alleviate symptoms of their condition or the discomfort caused by the equipment.
Contagious Diseases
If you have a contagious disease, you must be cared for in a separate area of the ICU. This is known as ‘isolation‘.
Staff and care teams in the ICU’s isolation section take extra precautions to keep infections under control. It is critical to prevent germs from infecting staff or other patients in the ICU.
Isolation may also be required if you have an infection that is difficult to treat. This can happen when bacteria become resistant to antibiotics.
Care after the ICU
Once the patient is discharged from the hospital, they will need a proper plan in place to ensure optimal recovery.
A great care plan will allow the patient to recover safely and comfortably while reducing the risk of avoidable hospital readmission.
NurseRegistry can help you or a loved one recover after a hospital stay.
We have California’s top nurses licensed in a variety of specialties of medical care. Our full range of services includes wound care, post-hospital care, airway management, and more.
From checking blood pressure to wound care and pain management, our private nurses offer high-end specialized care for a better quality of life.
Our nurses can provide high-quality care in the comfort of home for people of all ages. If you are being transferred to a nursing facility where you would like additional support, our nurses can provide supplemental care.
If you have any questions or would like to schedule services, click below today.
Frequently Asked Questions about the ICU
Is being in the ICU serious?
Intensive care is required if someone is critically ill and requires intensive treatment and close monitoring, or if they are having surgery and require intensive care to recover. Most ICU patients have problems with one or more organs. For example, they may be unable to breathe independently.
What is the chance of survival after ICU?
Overall, 76% of patients who spent more than 24 hours in the ICU were discharged alive from the hospital. During follow-up, the mortality rate among hospital survivors was 14.9% in the first year, rising to 20.5% after two years. Figure 3 shows the survival curves by age group.Feb 11, 2023
How long do patients normally stay in the ICU?
The average ICU stay was 10 to 25 days. The median length of stay was two days, with quarters ranging from one to seven days.
What does it mean when a patient is in the ICU?
An intensive care unit (ICU) provides critical care and life support to acutely ill and injured patients. Unless you are an emergency admission, you will require a referral from your doctor or specialist to be admitted to the ICU.
Can a family stay overnight in the ICU?
Some ICUs have limited provisions for relatives to stay overnight in exceptional circumstances. Some people had stayed overnight at the hospital, either because they lived a long distance away or because they wanted to be close to the patient.
Is ICU higher than Critical Care?
Intensive Care, also known as critical care, is a department in every acute hospital that treats critically ill patients. Critical care is typically divided into two units: the Higher Dependency Unit and the Intensive Care Unit (although they may share the same floor space).
Resources
ANZICS is an organization that offers advice and resources for patients who are going to be admitted into the ICU.
The Society of Critical Care Medicine offers guidelines, assistance, and grants to help patients and their families.
AICU consists of a group of doctors, former patients, and other healthcare professionals. They work together to provide ICU patients, families, and medical professionals with information on the road to recovery after a critical illness.