John visits his father, who resides in a nursing home, and is an invalid since his stroke left him incapacitated.
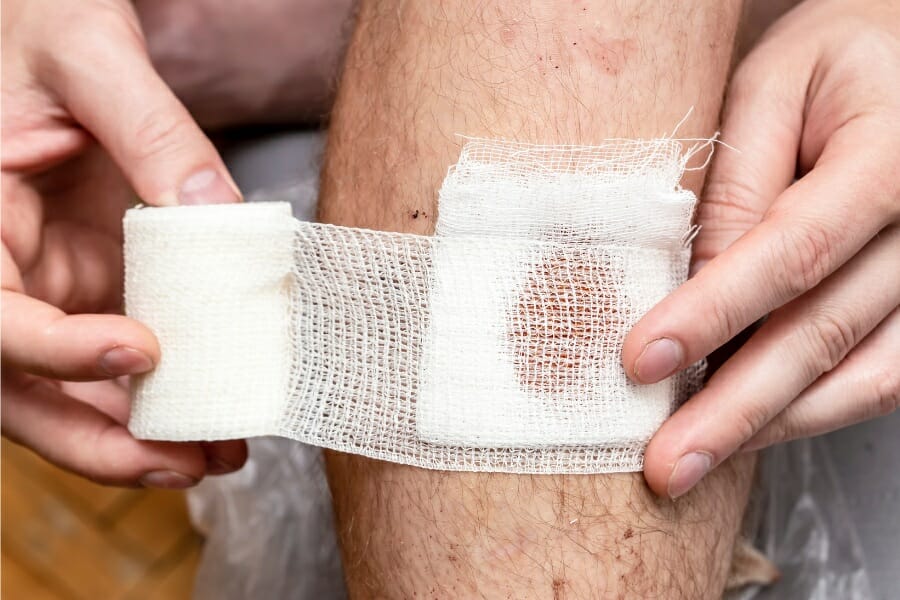
During one of his visits, he sees a large bandage on his father’s back, and subsequently sees a nurse change the dressing.
To his shock, he sees a large and raw wound that is cleaned by the nurse and then covered with a new dressing.
By the end of the day, John has not only given a piece of his mind to the manager of the nursing home but is considering moving his father to a new location as well as contacting authorities as well as an attorney to report elder abuse.
The Importance of Wound Care in Nursing Homes
IN THIS ARTICLE
Nursing homes play a crucial role in providing healthcare to the elderly population.
One of the most common health issues faced by residents in nursing homes is wounds.
Wound care is a critical aspect of nursing care in nursing homes, as it can prevent the development of infections and minimize the risk of hospitalization.
Wound Care and the Elderly While wound care is concerned with the treatment of surgical wounds, pressure and stasis ulcers, as well as problems with both bowel and urinary incontinence, it should be noted that the second leading cause of litigation in nursing homes is due to skin and wound allegations.
Wounds can be caused by a variety of factors, including pressure ulcers, surgical incisions, and injuries. Proper wound care can help prevent complications and promote faster healing. It is essential for nursing home staff to be trained in wound care to ensure that residents receive the best possible care.
It is not uncommon for legal claims against a facility in regard to wound care issues costing $250,000, and multiple wound care cases can make it difficult for a facility to obtain insurance, endangering both the patient’s as well as the facility’s livelihood.2
As a result, a jury will often find in favor of the plaintiff, when the appearance of incompetence or malpractice on behalf of the nursing home, due to the apparent indifferent treatment of the patient’s wound issues.3
As a result, the lack of a Certified Wound Care professional allows for the false perception that all facility-acquired wound problems are preventable.4
In fact, it has been proven repeatedly with statistically valid studies that properly trained nursing staff is one of the key factors in influencing patient safety and livelihood and reduced mortality.5
Wound Care Patient Demographics The most common wounds to be discussed are pressure ulcers (decubitus ulcers or bedsores), vascular ulcers (arterial and venous), and neuropathic ulcers.
Types of Wounds Common in Nursing Homes
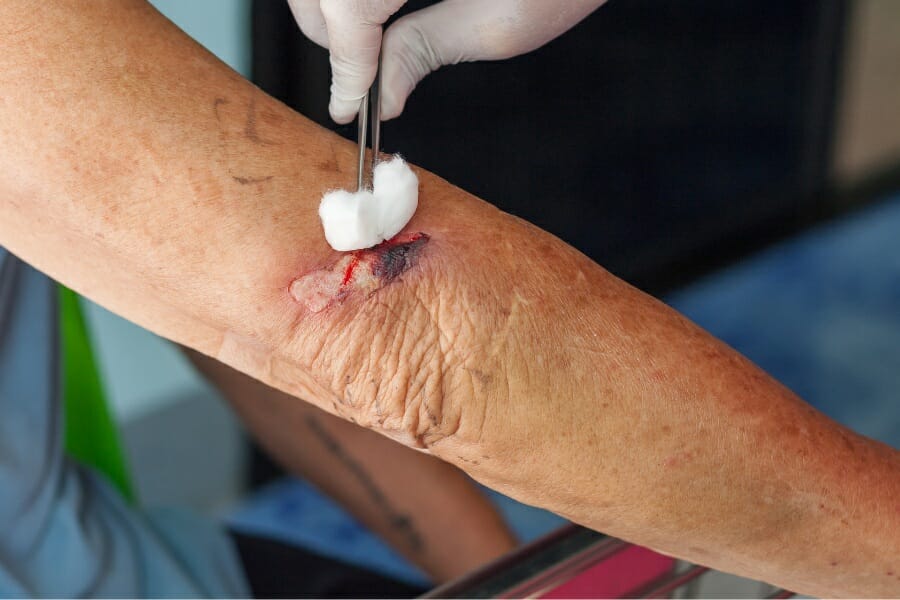
There are several types of wounds that are commonly seen in nursing homes. Pressure ulcers are one of the most common types of wounds, which are caused by prolonged pressure on the skin. Other types of wounds include surgical wounds, diabetic ulcers, and venous ulcers.
Pressure Ulcers Approximately 70% of all pressure ulcers occur in the geriatric population.
Their skin has a decrease in water content, tensile strength, and junctional integrity between the dermis and the epidermis. Atrophy of the apocrine and sebaceous glands causes drying of the skin.
A loss of subcutaneous tissue, vascularity, and diminishing stability of small blood vessels add other factors to compromise skin integrity.6
Pressure ulcers, also known as bed sores, pressure sores, or decubitus ulcers, are wounds caused by unrelieved pressure on the skin.7
They usually develop over bony prominences, such as the elbow, heel, hip, shoulder, back, and back of the head.8 Pressure ulcers are serious medical conditions and one of the important measures of the quality of clinical care in nursing homes.
The most common system for staging pressure ulcers classifies them based on the depth of soft tissue damage, ranging from the least severe (stage 1) to the most severe (stage 4).9 Approximately one out of every 10 nursing home residents (11%) had pressure ulcers.
- Residents aged 64 years and under were more likely than older residents to have pressure ulcers.
- Residents of nursing homes for a year or less were more likely to have pressure ulcers than those with longer stays.
- One in five nursing home residents with recent weight loss had pressure ulcers.
- Thirty-five percent of nursing home residents with stage 2 or higher (more severe) pressure ulcers received special wound care services in 2004.
Vascular ulcers result from deficits in either the quality of arterial flow or the derangement of the venous system.
The prevalence of peripheral arterial and peripheral venous disease is increased in the geriatric population.
The evaluation must include both systems because these problems are not mutually exclusive. Arterial ulcers are a result of restriction of flow or occlusion of an artery.
They have a discrete “punched out” appearance, a pale wound bed, and minimal exudate. Gangrene or necrotic tissue is common.
Due to the ischemia underlying the development of these ulcers, they are often very painful and difficult to treat or heal.10 The most frequent locations for these ulcers are the tips of or between the toes, over the phalangeal heads, or over the lateral malleolus.
Even a bump or scrape can precipitate an ulceration.11 Venous ulcers are generally shallow with irregular wound margins.
The ulcer base tends to be beefy red and granulation is frequent with exudates most often moderate to heavy. If there is an arterial component, the color and amount of exudates may be muted.
These wounds may have a strong odor that may be concerning to the patient and must be addressed when providing wound care. Venous ulcers are classically located over the medial malleolus although sometimes they can be near the lateral malleolus.
In severe cases, they may encircle the entire ankle. Other disease processes such as vasculitis, pyoderma gangrenosum, or neoplasms may be mistaken for venous ulcers.
Ulcers that do not respond to standard treatment should be referred for further evaluation, i.e., dermatology, vascular or plastic surgery.12
Neuropathic Ulcers Neuropathy is most often associated with diabetes, but may result from other diseases.
Neuropathy falls into three categories: sensory, motor, and autonomic. The most common is sensory neuropathy resulting in an insensate foot.
Ulcer causality is multifactorial, the presence of sensory neuropathy, peripheral occlusive vascular disease, and the presence of bony deformities increase the incidence of foot ulcers.13 Diabetic foot ulcers may be classified in stages according to the natural history progression:14
- Normal foot
- High-risk foot
- Ulcerated foot
- Infected foot
- Necrotic foot
Assessment and Management of Wounds
Nursing home staff must be able to identify the type of wound and provide appropriate wound care.
This includes cleaning the wound, changing dressings, and monitoring for signs of infection. In some cases, a wound care nurse may be needed to provide specialized care.
They should also provide appropriate management to promote healing and prevent complications. The following are some essential steps in wound assessment and management:
- Assess the wound type and depth: Identify the type and depth of the wound to determine the appropriate treatment plan.
- Clean the wound: Clean the wound with saline or other appropriate solutions to remove debris and bacteria.
- Debride the wound: Remove any dead or damaged tissue from the wound to promote healing.
- Apply appropriate dressings: Apply appropriate dressings to protect the wound and promote healing.
- Monitor for signs of infection: Monitor the wound for signs of infection, such as redness, swelling, and drainage.
- Provide pain management: Provide appropriate pain management to reduce discomfort and promote healing.
Wound Care Treatments
Wound care treatments vary depending on the type of wound and its severity. The following are some common wound care treatments used in nursing homes:
- Antibiotics: Antibiotics may be prescribed to treat infected wounds.
- Topical creams and ointments: Topical creams and ointments may be used to promote healing and reduce pain.
- Negative pressure wound therapy: Negative pressure wound therapy may be used to promote healing by removing excess fluid and promoting blood flow to the wound.
- Surgical interventions: Surgical interventions may be necessary for severe wounds that do not respond to other treatments.
Infection and Pain Management
Infection and pain management are critical components of wound care in nursing homes.
Nurses should monitor wounds for signs of infection and provide appropriate treatment to prevent complications.
They should also provide appropriate pain management to reduce discomfort and promote healing. The following are some essential steps in infection and pain management:
- Monitor for signs of infection: Monitor the wound for signs of infection, such as redness, swelling, and drainage.
- Provide appropriate antibiotics: Provide appropriate antibiotics to treat infected wounds.
- Provide appropriate pain management: Provide appropriate pain management, such as analgesics, to reduce discomfort and promote healing.
Prevention of Wounds in Nursing Homes
Prevention of wounds is critical in nursing homes to reduce the risk of complications and promote overall health and well-being.
Nurses should take the following steps to prevent wounds in nursing homes:
- Monitor residents regularly: Monitor residents regularly to identify any changes in their skin condition.
- Provide appropriate nutrition: Provide appropriate nutrition to promote overall health and well-being.
- Encourage mobility: Encourage residents to move and exercise regularly to promote circulation and prevent pressure ulcers.
- Use appropriate support surfaces: Use appropriate support surfaces, such as mattresses and cushions, to reduce pressure and prevent pressure ulcers.
The Process of Wound Healing
Wound healing is a complex process that involves the repair and restoration of damaged tissue.
The healing process can be divided into three distinct phases: inflammatory, proliferative, and remodeling. Each phase is characterized by a specific set of cellular and molecular events.
Inflammatory Phase
The inflammatory phase is the first stage of wound healing and begins immediately after tissue damage.
This phase is characterized by the release of inflammatory mediators such as cytokines and chemokines, which attract immune cells to the site of injury.
The immune cells remove debris and bacteria from the wound and initiate the process of tissue repair.
Proliferative Phase
The proliferative phase is the second stage of wound healing and is characterized by the formation of granulation tissue.
Granulation tissue is a new connective tissue that forms at the site of injury and is rich in blood vessels and fibroblasts. Fibroblasts are cells that produce collagen, a protein that provides strength and structure to the wound.
During this phase, the wound contracts as the edges pull together, reducing the size of the wound.
Remodeling Phase
The remodeling phase is the final stage of wound healing and can last for several months. During this phase, the newly formed tissue is remodeled and strengthened.
The collagen fibers are rearranged, and the wound becomes stronger and more resilient. The remodeling phase is also characterized by the maturation of the scar tissue.
Wound Care Challenges in Nursing Homes
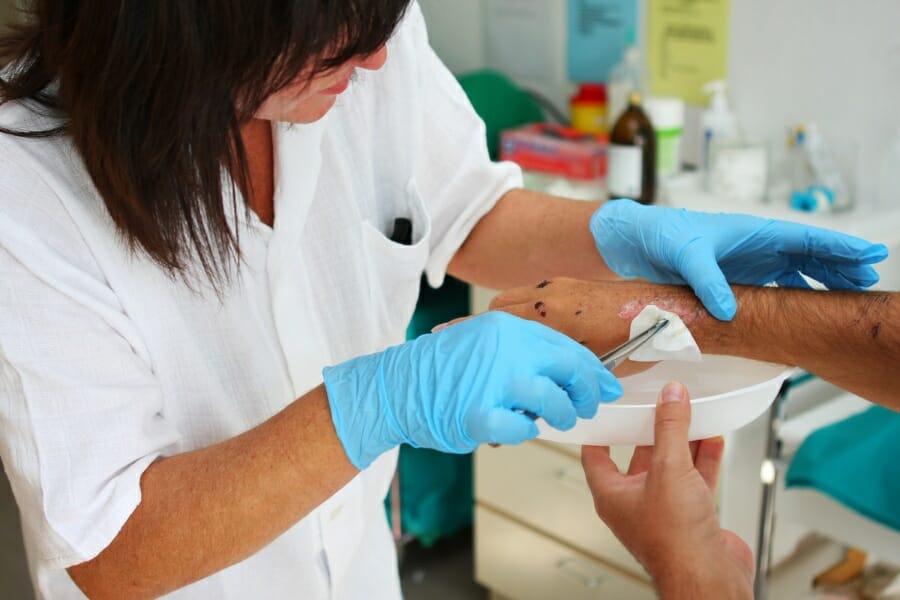
Staffing Issues
Nursing homes, long-term care facilities, and skilled nursing facilities often face staffing challenges that can impact the quality of wound care provided to patients.
A shortage of qualified nurses and other healthcare professionals can lead to inadequate monitoring and treatment of wounds.
In some cases, nursing homes may rely on untrained or undertrained staff to provide wound care, which can result in poor outcomes.
Lack of Training
Proper training is essential for healthcare professionals who provide wound care to nursing home residents.
Unfortunately, many nursing homes do not offer adequate training to their staff, which can result in improper wound care techniques and increased risk of infection.
In addition, healthcare professionals may not be aware of the latest wound care technologies and treatments, which can limit their ability to effectively treat wounds.
Patient Non-Compliance
Patient non-compliance can be a significant challenge in nursing home wound care. Patients in skilled nursing facilities may resist treatment or fail to follow wound care instructions, which can delay healing and increase the risk of infection.
Factors that can contribute to patient non-compliance include cognitive impairment, pain, and discomfort.
In addition to these challenges, nursing homes may also face issues with wound care documentation, communication between healthcare professionals, and access to specialized wound care products and services.
Addressing these challenges requires a multi-faceted approach that includes adequate staffing, ongoing training and education, and effective communication and collaboration among healthcare professionals.
Innovations in Wound Care
Role of Dressings and Topical Agents
Innovations in wound care have led to the development of advanced dressings and topical agents that promote healing and reduce the risk of infection.
These products are designed to provide a moist wound environment, which is essential for optimal healing. Some of the commonly used dressings include hydrocolloids, hydrogels, foams, and alginates.
Hydrocolloid dressings are made of gel-forming agents that absorb exudate from the wound and create a moist environment.
They are ideal for wounds with low to moderate exudate and can be used on partial or full-thickness wounds.
Hydrogels are another type of dressing that provides moisture to the wound bed and promotes autolytic debridement. They are ideal for dry or necrotic wounds and can be used on partial or full-thickness wounds.
Foam dressings are highly absorbent and provide cushioning to the wound bed.
They are ideal for wounds with heavy exudate and can be used on partial or full-thickness wounds. Alginate dressings are derived from seaweed and are highly absorbent.
They are ideal for wounds with heavy exudate and can be used on partial or full-thickness wounds.
Topical agents such as silver dressings, honey, and growth factors are also used in wound care. Silver dressings are used to reduce the risk of infection and promote healing.
Honey has antibacterial properties and promotes autolytic debridement. Growth factors such as platelet-derived growth factor (PDGF) and epidermal growth factor (EGF) promote cell growth and accelerate the healing process.
Advanced Techniques in Wound Care
In addition to advanced dressings and topical agents, there are several advanced techniques in wound care that have been developed in recent years.
Negative pressure wound therapy (NPWT) is one such technique that involves the use of a vacuum to promote healing. NPWT is used to treat chronic wounds, acute wounds, and surgical wounds.
Hyperbaric oxygen therapy (HBOT) is another advanced technique that involves the administration of oxygen at high pressure. HBOT promotes the growth of new blood vessels and accelerates the healing process. It is used to treat chronic wounds, radiation injuries, and other conditions.
Finally, there is the use of bioengineered skin substitutes, which are used to promote healing in chronic wounds.
These substitutes are made from living cells and can be used to replace damaged tissue. They are ideal for wounds that are difficult to heal and can be used on partial or full-thickness wounds.
Special Considerations for Specific Conditions
When it comes to wound care for elderly individuals, there are certain conditions that require special consideration.
We’ve already discussed pressure ulcers, here are some of the most common conditions and what to keep in mind when providing wound care:
Diabetes
Diabetes can impact wound healing and increase the risk of infection.
Patients with diabetes may have poor circulation and nerve damage, which can make it difficult for them to feel pain or notice a wound.
It is important to monitor blood sugar levels and work with a physician to develop a care plan that takes diabetes into account.
Peripheral Neuropathy
Peripheral neuropathy can also impact wound healing and make it difficult for patients to feel pain or notice a wound. Patients with peripheral neuropathy may require more frequent wound assessments and may need extra support to prevent further damage.
Moisture-Associated Skin Damage
Moisture-associated skin damage can occur when skin is exposed to moisture for an extended period of time. This can be a concern for patients who are incontinent or have wounds that require frequent dressing changes. It is important to keep skin clean and dry and to use appropriate dressings to prevent further damage.
Get Top Rated Wound Care
Whether you have an elderly loved one that needs wound care or you run a healthcare facility that needs exceptionally trained and professional nurses, NurseRegistry can help.
With over 500 nurses, we can guarantee to provide you with a high-end RN or LVN who has extensive wound care skills and experience.
Click below to learn more about NurseRegistry today.
Frequently Asked Questions
What is nursing home wound care?
Wound care nursing is a specialized field that focuses on the assessment, treatment, and prevention of wounds.
Wound care nurses work with patients who have acute or chronic wounds, including pressure ulcers, surgical wounds, and diabetic foot ulcers.
They use a variety of techniques and tools to promote healing and prevent infection.
What are the best practices for wound care?
The best practices for wound care involve a comprehensive approach that includes proper assessment, treatment, and prevention strategies.
This includes regular monitoring of wounds, cleaning and dressing wounds appropriately, and addressing any underlying health issues that may be contributing to the wound.
Wound care nurses should also have a thorough understanding of the latest research and best practices in wound care.
What are the most common types of wounds in nursing homes?
The most common types of wounds in nursing homes are pressure ulcers, also known as bedsores.
These are caused by prolonged pressure on the skin and can be prevented by regular repositioning and skin care. Other common types of wounds in nursing homes include surgical wounds, diabetic foot ulcers, and venous ulcers.
How can nursing homes ensure proper wound care for their residents?
Nursing homes can ensure proper wound care for their residents by implementing a comprehensive wound care program that includes regular assessment, treatment, and prevention strategies.
This may involve training staff on proper wound care techniques, providing appropriate equipment and supplies, and working closely with wound care specialists.
What are the potential complications of improper wound care in nursing homes?
Improper wound care in nursing homes can lead to a range of complications, including infection, delayed healing, and even amputation in severe cases.
It can also lead to pain and discomfort for residents, and can have a negative impact on their overall quality of life.
What resources are available for nursing homes to improve their wound care practices?
There are a variety of resources available for nursing homes to improve their wound care practices, including training programs for staff, wound care specialists who can provide guidance and support, and online resources such as wound care guidelines and best practices.
Nursing homes can also work with their local healthcare community to develop partnerships and collaborations that can help improve wound care outcomes for their residents.
References 1Chizek, Margaret, “Wound Care and Lawsuits,” Advance Healthcare Network for Nurses, Volume 5, Issue 7, page 31, March 17, 2003.
2O’Conner, John, “Documentation is critical in wound care lawsuits: expert,” McKnight’s, May 1, 2012.
3Fowler, Elaine, “Deposed: A Personal Perspective,” Legal Issues in the Care of Pressure Ulcer Patients: Key Concepts for Healthcare Providers, Medline.
4Caroline E. Fife, MD, & Kevin Yankowsky, JD, “Avoiding Legal Pitfalls for Home Health Services in Wound Care,” Today’s Wound Clinic, Volume 7, Issue 4, May 2013.
5Van den Heede, K., “The relationship between inpatient cardiac surgery mortality and nurse numbers and educational level: Analysis of administrative data,” International Journal of Nursing Studies, 2009 Jun; 46(6): 796–803.
6 Thomas DR. Issues and dilemmas in prevention and treatment of pressure ulcers: a review. J Gerontol. 2001;56A:M328–M340.
7 Agostini J, Baker D, Bogardus Jr S. Prevention of pressure ulcers in older patients. In: Shojania K, Duncan B, McDonald K, et al., eds. Making health care safer: A critical analysis of patient safety practices Evidence Report/Technology Assessment No. 43, AHRQ Publication No. 01-E058. Rockville, MD: Agency for Health Care Research and Quality, 2001.
8Cuddigan J, Berlowitz DR, Ayello EA. Pressure ulcers in America: Prevalence, incidence and implications for future: An executive summary of the National Pressure Ulcer Advisory Panel Monograph. Advances in Skin & Wound Care 14:208-15. 2001.
9 Institute of Medicine. Improving the quality of long-term care. Washington, DC: National Academy Press, 2001.
10 Paquette D. Leg ulcers. Clinics Geri Med. 2002;18:77–88.
11 Wipke-Tevis DD. Management of vascular leg ulcers. Adv Skin Wound Care. 2005;18:437–445.
12 Brill LR. New treatments for lower extremity ulcers. Patient Care for the Nurse Practitioner. 2001;12:9–20.
13 Kravitz SR. The treatment of diabetic foot ulcers: Reviewing the literature and a surgical algorithm. Adv Skin Wound Care. 2007;20:227–237.
14 Edmonds M. A natural history and framework for managing diabetic foot ulcers Br J Nurs 200817S20, S22,S24–S29.S29 15 Mulder GD. Management of the diabetic foot ulcer in the elderly population. Clin Geriatrics. 2003;11:46–53.
16 Inlow S. Best practices for the prevention, diagnosis and treatment of diabetic foot ulcers. Ostomy Wound Manage. 2000;46:55–68.
17 Nursing home enhanced quality measures, Centers for Medicare and Medicaid Services.
182007 Home Health Line’s PPS Benchmarks Handbook, 6th Edition. Rockville, Md., 2007.
19Poliey, Lorraine, “The Benefits of Dedicated Home Nursing for Treating Wounds,” Harvard Business Review, September 19, 2013.
20 Zaratkiewicz, S., “Development and Implementation of a Hospital-Acquired Pressure Ulcer Incidence Tracking System and Algorithm,” Journal of Healthcare Quality, 2010, Nov-Dec, 32(6), pp. 44-51.
21 Kendall-Gallagher D. Aiken LH. Sloane DM. Cimiotti JP., “Nurse specialty certification, inpatient mortality, and failure to rescue,” Nurse Scholarship, 2011;43:188.
22 Zulkowski K, et al. “Certification and education: do they affect pressure ulcer knowledge in Nursing? “Advanced Skin and Wound Care Journal, 2007;20:34.
23 Henderson-Everhardus MC. “Does nursing expertise contribute to the accuracy of vascular assessment in the detection of peripheral arterial disease?” Texas Woman’s University; Denton, Texas: 2004.
24Westra, Bonnie, “Effectiveness of Wound, Ostomy, and Continence Nurses on Agency-Level Wound and Incontinence Outcomes in Home Care,” Journal of Wound Ostomy Continence Nursing, 2013;40(1):25-33.






