What kind of risk does it pose? According to the CDC, 1 in 3 people will develop shingles in their lifetime and approximately half of these cases occur in patients over 60.
With the older population at such a high risk and those who may already be experiencing health issues, it is vital for caregivers to know how to care for a patient with shingles and to be aware of complications that can arise.
What is Shingles?
IN THIS ARTICLE
Shingles, also known as herpes zoster, is a viral infection caused by the varicella-zoster virus.
This is the same virus that causes chickenpox. After a person recovers from chickenpox, the virus remains dormant in the body’s nervous system. Later in life, the virus can reactivate and cause shingles.
The symptoms of shingles typically include pain, burning, or tingling on one side of the body, along with a red rash that may blister. The rash usually appears in a band or strip, following the path of the affected nerve. Other symptoms may include fever, headache, and sensitivity to light.
Shingles is not contagious, but the varicella-zoster virus can be spread from a person with shingles to someone who has never had chickenpox. In this case, the person may develop chickenpox, but not shingles.
There is no cure for shingles, but antiviral medication can help reduce the severity and duration of symptoms.
Pain relief medication may also be prescribed to manage the discomfort associated with shingles. It is important to seek medical attention as soon as possible if shingles is suspected, as early treatment can help prevent complications and reduce the risk of long-term pain.
Cause and Symptoms
Shingles is caused by a reactivation of the herpes zoster virus, which is the same virus that causes chicken pox. It manifests itself in the form of a painful skin rash that can last up to four weeks. The pain can be described as aching, burning and even stabbing. This can be very debilitating and affect the quality of life to the point of :
- Depression
- Anxiety
- Difficulty Concentrating
- Loss of Appetite
- Weight Loss
Shingles can also interfere with daily activities such as :
- Dressing
- Bathing
- Meal Preparation
- Eating
- Shopping
- Mobility
- Sleep
Let’s go into a little more detail about some of the symptoms and causes often associated with shingles.
Symptoms of Shingles
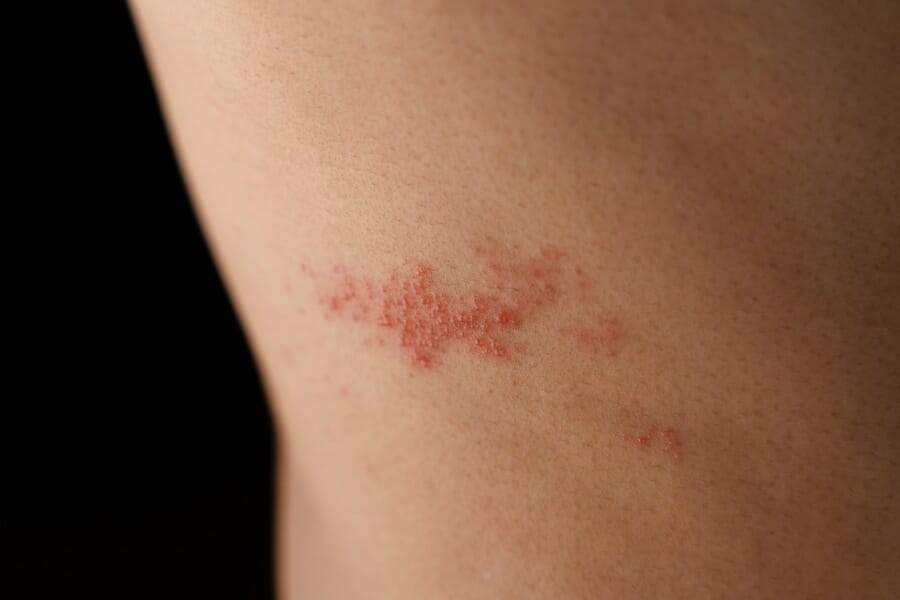
Shingles is a viral infection that causes a painful rash. This is one of the most common side effects.
The symptoms of shingles can vary from person to person, but they typically include pain, burning, and tingling in a specific area of the body. In this section, we will discuss the various symptoms of shingles.
Initial Symptoms
The initial symptoms of shingles can include a general feeling of fatigue, fever, and headache. Some people may also experience tingling, burning, or sensitivity to touch in the affected area. These symptoms can last for several days before the rash appears.
Los of Appetite due to Shingles
It is commonly reported that folks with shingles will experience a loss of appetite. This goes along with fatigue and sluggishness which is common before any severe pain symptoms of shingles.
Rash and Blisters
The most common symptom of shingles is a painful rash that develops on one side of the body. The rash usually appears as a band or stripe of red, fluid-filled blisters that break open and crust over. The rash can be accompanied by itching, burning, and sensitivity to touch. The rash typically lasts for 2-4 weeks.
Postherpetic Neuralgia
After the rash has healed, some people may experience a complication known as postherpetic neuralgia (PHN). PHN is a type of nerve pain that can last for months or even years after the rash has healed. The pain can be severe and debilitating, and it can make it difficult to perform daily activities.
Eye Involvement
Shingles can also affect the eye, causing a condition known as herpes zoster ophthalmicus (HZO). HZO can cause eye pain, redness, swelling, and vision loss. In severe cases, it can even lead to permanent damage to the cornea and vision loss.
Other Symptoms
In addition to the symptoms mentioned above, some people may experience other symptoms during a shingles outbreak. These can include chills, swelling, and general body aches. In rare cases, shingles can also cause hearing loss, facial paralysis, or inflammation of the brain.
Causes and Risk Factors of Shingles
Shingles is caused by the reactivation of the varicella-zoster virus, which is the same virus that causes chickenpox.
After a person recovers from the chickenpox virus, the virus remains dormant in the nervous system. Later in life, the virus can reactivate and cause shingles. The exact reason why the virus reactivates is not clear, but there are several factors that can increase the risk of reactivation.
Therefore, shingles is not a result of an adult coming in direct contact with another individual who is suffering from shingles.
One of the primary risk factors for shingles is age. The risk of developing shingles increases as a person gets older, with the highest incidence in people over 50 years old. This is because the immune system weakens as people age, making it more difficult for the body to fight off infections.
A weakened immune system is another significant risk factor for shingles. People with weakened immune systems due to illnesses like cancer, HIV, or those undergoing chemotherapy are more likely to develop shingles. This is because the immune system is responsible for keeping the virus dormant, and when it is weakened, the virus can reactivate.
Stress is another factor that can increase the risk of shingles. Stress weakens the immune system, making it more likely for the virus to reactivate. People who are under a lot of stress, either from work or personal life, are more likely to develop shingles.
Other risk factors for shingles include:
- Having had chickenpox before the age of one
- Having a family history of shingles
- Being female
- Taking medications that weaken the immune system, such as steroids
In conclusion, shingles is caused by the reactivation of the varicella-zoster virus, which can be triggered by several factors, including age, a weakened immune system, and stress. It is essential to understand the risk factors for shingles to take steps to prevent the virus’s reactivation.
Diagnosis of Shingles
Diagnosing shingles can be done by a healthcare provider. The doctor will start by asking about the patient’s medical history and symptoms. They will also examine the patient’s rash and blisters.
In some cases, the doctor may take a tissue sample or culture of the blisters to send to the lab for testing. This can help confirm the diagnosis of shingles and rule out other conditions with similar symptoms.
It’s important to seek medical attention as soon as possible if shingles is suspected. Early diagnosis and treatment can help reduce the severity of symptoms and prevent complications.
In some cases, shingles can be difficult to diagnose, especially in its early stages. This is because the symptoms can be similar to other conditions, such as eczema or hives. A doctor may need to conduct additional tests or refer the patient to a specialist for further evaluation.
Overall, a prompt diagnosis is crucial for effective treatment of shingles. If you suspect you may have shingles, it’s important to see a doctor as soon as possible to get an accurate diagnosis and begin treatment.
Treatment and Management of Shingles
Shingles is a viral infection that causes a painful rash and blisters. While there is no cure for shingles, early treatment can help speed up the healing process and reduce the risk of complications. This section will cover the different treatment options available for managing shingles.
Medications
Antiviral medications are often prescribed to treat shingles. These drugs work by stopping the virus from multiplying, which can help reduce the severity and duration of symptoms. Common antiviral medications used to treat shingles include acyclovir, famciclovir, and valacyclovir.
In addition to antiviral medications, pain medications may also be prescribed to help manage the discomfort associated with shingles. These may include over-the-counter pain relievers such as acetaminophen or ibuprofen, as well as prescription-strength pain medications like opioids.
Pain Management
Shingles can be a very painful condition, and managing pain is an important part of treatment. In addition to pain medications, there are other strategies that can help alleviate discomfort. These may include:
- Applying cool compresses to the affected area
- Taking a cool bath or shower
- Using topical creams or ointments that contain capsaicin
- Using numbing agents such as lidocaine
There are many conditions that may cause alarm for elderly individuals, such as pneumonia, and shingles is very similar.
It is important to talk to a healthcare provider about the best pain management strategies for individual cases of shingles.
“Acute pain should… be treated starting with acetaminophen and increasing the analgesic effect as needed to include codeine, oxycodone, and morphine, depending on the effectiveness of treatment, severity of pain, and side effects of the analgesics.” (MHC)
It is also important to consider the other medications the patient may be taking and how these analgesics could interact with them. Caregivers should be sure to look for adverse side effects to analgesics including constipation, urinary retention, dry mouth, or confusion.
If the patient is unable to tolerate a high dose of opioid pain medication, the lowest effective dose should be used in conjunction with other pain management therapies (MHC).
In addition, an in-home nurse can assist individuals suffering from shingles with pain management care.
Complications
Postherpetic Neuralgia or PNH is the most common complication of shingles and is a continuation of the pain after the rash itself has healed. Age increases the risk. The severity of the pain can remain and is treated with medication ranging from painkillers to anti-seizure medication to skin creams (Iliades)
Bacterial infections are another complication to be aware of. The shingles rash presents as a blister that ruptures. Once ruptured, bacteria can get into the sore and cause an infection, most commonly as a result of scratching. (Iliades) Bacterial infections are treated with antibiotics.
Blurry vision or even vision loss can also occur. If the patient has pain on one side of the face or a rash on the tip of the nose, this is a sign that the infection may be spreading to the eye. If the patient has decreased vision, eye pain or discomfort, eye redness, or sensitivity to light or eye swelling, the patient should see an eye doctor right away to prevent serious complications. Antiviral medication can be prescribed in this situation. (Iliades)
Ramsey Hunt Syndrome is a complication where shingles attack the facial nerves. This presents as a rash on one side of the face, ear pain, or facial drooping. The patient may also complain of dizziness, loss of hearing, ringing in the ears, or loss of taste. These symptoms may be permanent, but most cases clear up after a combination of antivirals and steroids. (Iliades)
Herpes Zoster Encephalitis is a rare but very serious complication occurring when the virus enters the brain. This leads to a swelling of the brain requiring hospitalization and a combination of IV medications. Symptoms start quickly and include confusion, headaches, vomiting, and fever. (Iliades)
Preventing Complications
While shingles typically resolves on its own, complications can sometimes arise. These may include postherpetic neuralgia, a condition in which pain persists even after the rash has healed, or bacterial infections of the skin. To help prevent these complications, it is important to:
- Keep the affected area clean and dry
- Avoid scratching or picking at the blisters
- Wear loose-fitting clothing to avoid irritation
- Avoid close contact with individuals who have not had chickenpox or the chickenpox vaccine
In some cases, a healthcare provider may also recommend the use of steroids to help reduce inflammation and prevent complications.
Overall, treatment and management of shingles involves a combination of medications, pain management strategies, and preventative measures. It is important to work closely with a healthcare provider to determine the best course of treatment for individual cases.
Prevention of Shingles
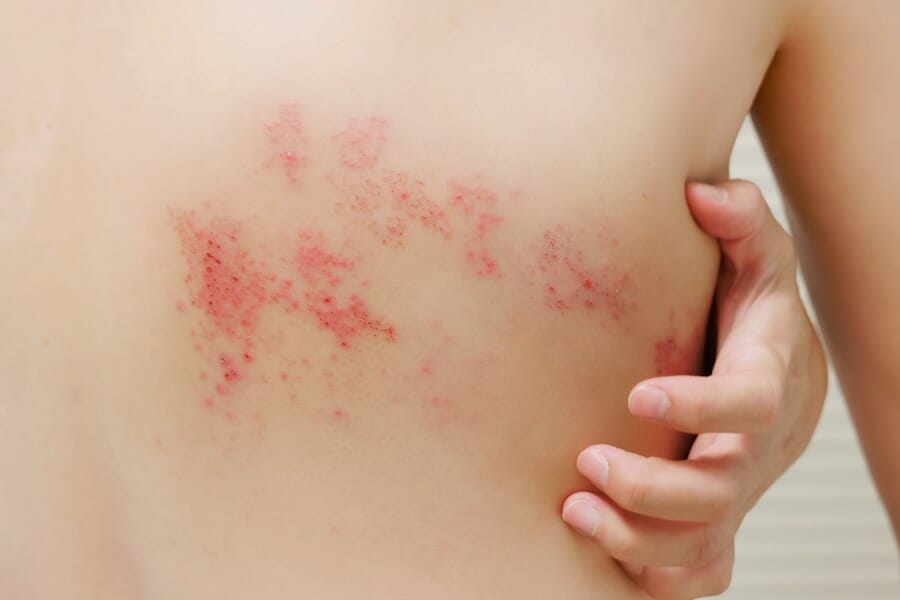
Shingles can be prevented through vaccination.
The CDC recommends that adults over the age of 50 receive the Shingrix vaccine, which is more than 90% effective at preventing shingles. This shingles vaccine is given in two doses, two to six months apart. It is also recommended for individuals who have previously received the Zostavax vaccine.
The Shingrix vaccine is a non-live vaccine that contains a protein from the varicella-zoster virus. It is recommended for healthy adults over the age of 50, including those who have previously had shingles or received the Zostavax vaccine. However, individuals with weakened immune systems or those who are allergic to any of the vaccine components should not receive the Shingrix vaccine.
It is important to note that the Shingrix vaccine may cause side effects, such as pain and swelling at the injection site, headache, and fatigue. These side effects are usually mild and go away on their own within a few days.
In addition to the shingles vaccine, there are other ways to prevent shingles. Good hygiene practices, such as washing hands frequently and avoiding contact with individuals who have active shingles, can help prevent the spread of the virus. It is also important to maintain a healthy immune system through regular exercise, a balanced diet, and adequate sleep.
Living with Shingles
Living with shingles can be difficult due to the pain and discomfort caused by the rash. It is important to understand the triggers that can cause shingles outbreaks. Common triggers include stress, illness, and a weakened immune system.
One of the most common symptoms of shingles is itchy skin. Caregivers can help alleviate this symptom by preparing colloidal oatmeal baths or gently spreading calamine lotion on the affected area. It is also important to avoid scratching the rash as it can lead to infection.
Shingles affects the nerves and can cause sensitivity to touch. Caregivers should be aware of this and take precautions when caring for someone with shingles. They should avoid touching the rash and wash their hands frequently to prevent the spread of the virus.
It is important to note that shingles is contagious and can be spread to those who have not had chickenpox. Caregivers should take precautions and avoid contact with those who have not had the chickenpox vaccine.
Living with shingles can be challenging, but with proper care and management, symptoms can be alleviated. It is important to seek medical treatment and follow the advice of healthcare professionals.
Care Tips for Shingles
Monitor medication compliance. “The risk of patient nonadherence increases with the more times per day a drug is dosed.” (MHC) Make sure the patient is taking every dose, every day. If pain is being controlled with NSAIDs, make sure they are being administered around the clock.
Be observant for medication side effects. Consider a prophylactic laxative to prevent constipation. (MHC) Also, be aware of medications the patient may be taking regularly to treat other issues to make sure there are no adverse reactions between those and the required medications to treat the shingles outbreak.
Practice good wound care of lesions to avoid infection. Caregivers should always wear gloves to prevent the spread of bacteria to the patient and the spread of the virus. Wounds should be carefully cleaned with mild soap and warm water. Good hand washing must also be practiced.
Watch for signs of complications and seek treatment immediately if any should occur.
Get Exceptional Shingles Care at Home
If you or a loved one has shingles, a private duty nurse can help with pain management, medication management, wound care, and other skilled services. Elderly loved ones do not have to deal with the pain symptoms on their own or need to relocate to a medical facility.
Instead, professional and knowledgeable nurses can assist with pain management and care every step of the way. This peace of mind, for both patients and their loved ones, can be pivotal during this severe condition.
Click below to learn more about how an in-home nurse from NurseRegistry could benefit your loved one suffering from shingles today.
Frequently Asked Questions
What are the early symptoms of shingles?
Early symptoms of shingles include pain, itching, or tingling on one side of the body or face. Some people may also experience fever, headache, and sensitivity to light. A rash may also appear, which can develop into fluid-filled blisters that scab over and eventually heal.
What causes shingles to activate?
Shingles is caused by the varicella-zoster virus, which also causes chickenpox. After a person recovers from chickenpox, the virus remains dormant in the nervous system. Shingles can occur when the virus reactivates later in life due to a weakened immune system or stress.
Is shingles dangerous?
Shingles can cause pain, itching, and discomfort, but it is usually not dangerous. However, in some cases, shingles can lead to complications such as nerve pain that continues after the rash clears up, vision loss, or skin infections.
How long does shingles pain last?
Shingles pain can last for several weeks or months, even after the rash has healed. Pain management techniques such as over-the-counter pain relievers or prescription medications may help alleviate discomfort.
What helps shingles heal faster?
There is no cure for shingles, but antiviral medications can help reduce the severity and duration of symptoms. Pain management techniques such as cool compresses, calamine lotion, and colloidal oatmeal baths may also help alleviate discomfort and promote healing.
How long should you stay home with shingles?
People with shingles should avoid contact with individuals who have not had chickenpox or the chickenpox vaccine, as shingles can be contagious. It is recommended that individuals with shingles stay home until the rash has healed and the blisters have scabbed over.
Sources
“Prevent Shingles.” Centers for Disease Control. https://www.cdc.gov/features/shingles/
Iliades, Chris. “5 Complications of Shingles.” Healthgrades. https://www.healthgrades.com/conditions/5-complications-of-shingles
“Ask the Expert: Managing Shingles in Older Adults.” Managed Healthcare Connect. March 14, 2014. http://www.managedhealthcareconnect.com/article/managing-shingles–older-adults-ask-the-expert







